This blog is about myofascial trigger points
Have you ever had strong shooting pain in your buttocks or your neck? A pain that makes you sweat and your heart beat faster?
Those could be symptoms of a trigger point.
Still, a myofascial trigger point doesn’t always provoke discomfort. Sometimes you only feel that one muscle tires quicker than others. Or you notice a lack of coordination in your right ankle compared to your left.
This can greatly influence your sports performance.
Luckily though, myofascial trigger points are easy to treat. And with the right knowledge, you can spot them before they become a problem.
That’s why in this blog you’ll discover what a myofascial trigger point is. How you find them in your muscles, and what happens on a microscopical level. In the end, you’ll find general recommendations to prevent and to treat myofascial hypertension.
- What is a Myofascial Trigger Point?
- What are the Symptoms of a Trigger Point?
- How do Myofascial Trigger Points Come into Being?
- Where are Myofascial Trigger Points?
- How can Trigger Points Reduce your Sports Performance?
- What is Trigger Point Therapy?
- General Prevention of Hypertension
- Important Take-Aways
1. What is a Myofascial Trigger Point?
Before we jump on to the definition of a trigger point, I believe it’s good to know what “myofascial” means. As things go, in the scientific literature, trigger points are often described as “myofascial trigger points”.
Myofascial means muscle (myo) and connective tissue (fascia). Thus, a trigger point is found in the muscle and connective tissue.
Now on to the official definition of a trigger point:
A myofascial trigger point is a hyperirritable spot within a taut band of skeletal muscle that is painful on compression, stretch, overload, or contraction of the tissue which usually responds with a referred pain that is perceived distant from the spot.[i]
Right of the bat, even though trigger points were first described in 1999 there’s still no agreement on what the (real) origin of a trigger point is. Some argue the above, others that it’s a neurologic dysfunction1, and again others argue it’s a muscle spindle dysfunction.2
Does all of this matter for you – someone that wants to use smart techniques to increase sports performance?
I believe not.
Why?
Because both as a Physical Therapist treating clients with myofascial trigger points and as someone that uses self-myofascial release techniques – I found that it’s possible to release trigger points and that it reduces pain and discomfort.
More on the effects of trigger points on sports performance further on in this article.
First, let’s have a look at how you identify trigger points.
2. What are the Symptoms of a Trigger Point?
There are 2 types of myofascial trigger points:
- Active. A trigger point you feel without actively provoking it. This type of hypertension can be the source of your back or shoulder pain for example.
- Passive. A passive or latent myofascial trigger point only produces pain when you provoke it. For example, if you start pressing into your calf muscle right now there’s a chance, you’ll find a tender spot that produces a radiating pain. This would be a passive trigger point.
Both active and passive myofascial trigger points have similar symptoms:
- They produce sharp or dull pain
- The pain can be felt in another place than where the trigger point is at
- In the case of an active trigger point, when you press into a muscle the tender spot produces a familiar pain
- When pressing into a muscle you notice a tout band within a muscle fiber
3. How do Myofascial Trigger Points Come into Being?
Myofascial trigger points are a symptom of overuse. This can be due to mechanical overuse like doing a lot of sports, sitting for prolonged periods, or lifting using bad technique.
Besides that, stress can also cause an increase in muscle tension which in turn can lead to myofascial trigger points.
At the site of a trigger point, there’s a different chemical balance than in places without them.3 For example, chemicals like substance P and TNF-alpha.4 These are chemicals that you otherwise find at the site of an inflammatory response. Say, due to a cut in your arm or a torn muscle.
Thus, on a microscopical level, there’s an inflammatory response and a lack of bloodflow (ischemia) in a muscle fiber. This provokes nerve endings and sends a pain signal to your brain. While at the same time, the trigger point prohibits normal blood flow. As a result, the inflammatory chemicals can’t be absolved by regular blood flow. This, in turn, leads to continuous stimulation of pain receptors.
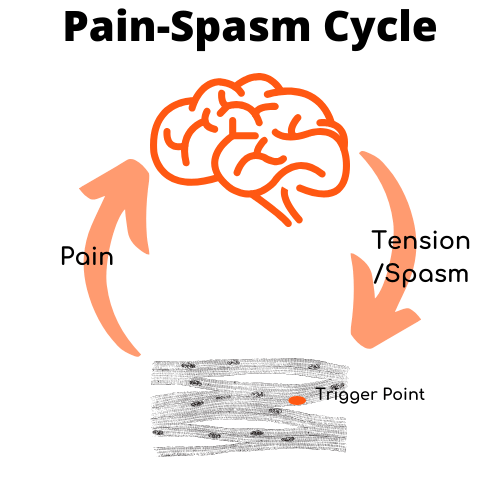
Do you see how this is a vicious cycle?
The inflammatory chemicals provoke pain. The brain notices the pain and tenses the muscles in return. This makes it even harder to clear out the chemicals which results in more stimulation of pain receptors. Which your brain responds to, again, with an increase in muscle tension.
Now you know what is a trigger point.
Let’s see where you can find them throughout the body.
4. Where are Myofascial Trigger Points?
Trigger points can be found in every muscle of the body.
As a rule of thumb, mostly at a third or at two-thirds of the length of a muscle.
These are common places where you find myofascial tension:
Levator Scapulae Muscle
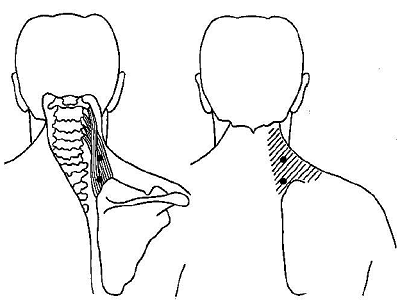
Trapezius Muscle (Ascending Part)
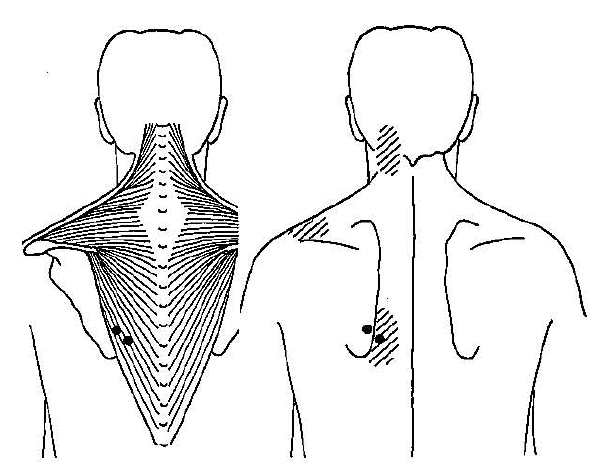
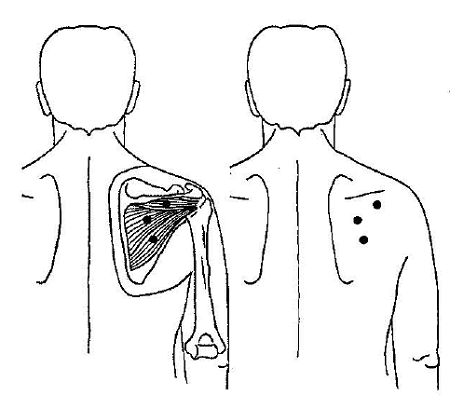
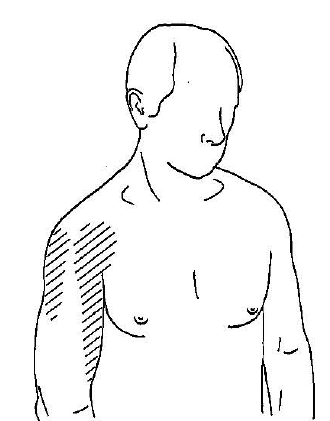
Infraspinatus Muscle (Rotator Cuff)
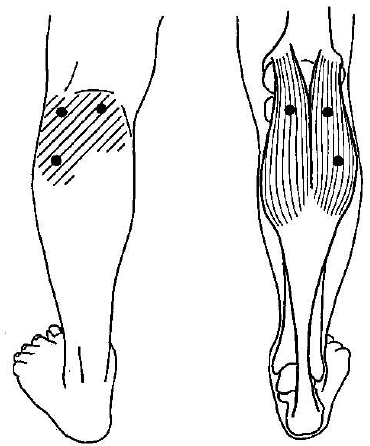
Gastrocnemius Muscle (Calf Muscle)
Gluteus Medius Muscle
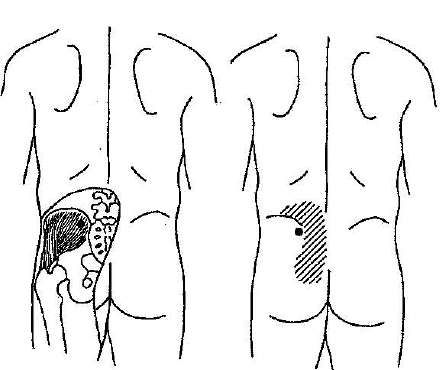
Do you see the striped areas?
These are the pain radiation patterns of that specific trigger point.
In fact, most of the trigger points have predictable pain patterns. Thus, a good Physical Therapist will, for example, always check for tension and trigger points in your rotator cuff when you have pain in your elbow.
I believe that you now have a solid idea about what is a trigger point and where to find them.
5. How can Trigger Points Reduce your Sports Performance?
As I mentioned at the beginning of this article trigger points can be categorized as “active” and “passive”.
An active trigger point will cause spontaneous pain. Logically, this will stimulate you to do something about it and resolve your pain and discomfort.
Even though passive trigger points behave differently than active ones, they do have the capacity to inhibit your physical performance.
3 Signs Latent Myofascial Trigger Points are Reducing your Sports Performance
1. Quickly Fatigued Muscles
It turns out that muscles that contain latent trigger points show signs of fatigue earlier on electromyographic (EMG) recordings than muscles that don’t.5
Moreover, it seems that the motor units innervating these muscles overload quicker. Motor units are the nerve endings that connect nerve and muscle. The better motor units work the more force you can generate, the better your coordination, and the longer it takes for you to tire.
2. Muscle Cramps
Muscle cramps are a common sign of overuse. One of the ways cramps occur is increased pain sensitivity in that area.
That’s why researchers used glutamate injections to provoke pain in latent myofascial trigger points. They also injected the same substance in areas that were free of trigger points. Besides that, to confirm that it was not just the injection, they also injected a salt-water solution into latent trigger points.
They found that in 92.86% of the cases where they injected glutamate into a latent trigger point they measured cramp with an EMG. They didn’t record any cramp-like reactions when they injected into non-trigger point sites or while injecting the saline solution into either one of the areas.6
This way the researchers showed that trigger points may play a significant role in the origin of cramps.
3. Altered Patterns of Muscular
The third sign of latent trigger points reducing your sports performance is due to altered muscle activity.7
During an isometric contraction (flexing a muscle without moving, like when you press against a wall or staying in a half-squat position), the researchers found, that the opposite (the antagonist) to the working muscle didn’t fully relax.

This is essential for generating maximum force and coordination.
To explain this phenomenon, can you extend your knee?
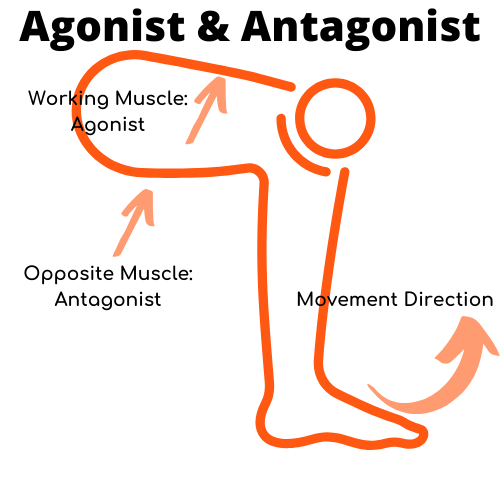
If you’re sitting you move your foot from the floor until your leg is straight. Your quadriceps (the muscle on top of your upper leg) is responsible for this movement. But for your quadriceps to efficiently make this movement your hamstrings (the muscles at the back of your leg) need to relax. It seems that trigger points reduce the amount the hamstring relaxes in this case.
As a result, your quadricep needs to work harder because the hamstring isn’t “letting go”.
6. What is Trigger Point Therapy?
Trigger points can be released (manually) in two different ways:
- Manual Friction Massage
- Dry Needling
Often combined with stretching in between, and at the end of releasing the myofascial trigger point.
In the case of manual friction massage, a therapist will apply pressure on the trigger point to increase blood flow to the area. In between pressing for 30-60 seconds, it’s a good idea to stretch the affected muscle. This way you help restore range of motion and support blood flow even more.
In the case of dry needling, a therapist will insert a needle right into the myofascial trigger point. The purpose is similar to that of friction massage.
In research where they looked if dry needling or manual massage was more efficient for neck and shoulder pain there was no difference between the two strategies. Both seemed to work equally well.8
7. General Prevention of Hypertension
Hypertension is an increase in muscle tone due to over or underuse. Your muscles can be tense with or without trigger points.
Yet, an active myofascial trigger point always provokes hypertension in a muscle. Remember the pain-spasm cycle typical for a trigger point?
That’s why general preventive strategies for hypertension are a great way to reduce the chance of myofascial trigger points.
Consider these strategies:
- Do a thorough warming-up before each time you do sports
- Do a thorough cool-down after each time you do sports (run at least 10-15 minutes at 40-50% of your max heart rate where after you finish with 30-60sec stretching of the muscles you used during your sport)
- A regular sports massage can help reduce muscle tone
- Apply self-myofascial release to mimic trigger point therapy with a tennis ball or foam roller
- Take sufficient rest between separate training moments to give your body time to remove lactate from the muscles and replenish them with glycogen
8. Important Take-Aways
This blog looked at myofascial trigger points, where you can find them throughout the body, and how they come into being. Moreover, you now know that trigger points can affect your sports performance.
Thus, it’s a good idea to manage the intensity of your sport by taking sufficient rest days. In this manner, you’ll reduce the chance of overload symptoms like hypertension in your muscles and connective tissue.
Besides going for a (preventive) sports massage, dry needling or manual friction can reduce trigger point symptoms.
Moreover, you can mimic trigger point therapy by using a tennis ball or a foam roller. In next week’s blog, I’ll explain how to do self-myofascial release to improve your flexibility, reduce pain levels, and improve sports performance.
Now I’d like to ask you. Have you ever had a trigger point? Where did it occur and how did you make it go away? Let me know in the comments below.
Citations
[i] Simons DG, Travell JG, Simons L. Myofascial Pain and Dysfunction. The Trigger Point Manual. 3th ed. Philadelphia: Wolters Kluwer; 2019
- Quintner JL, Bove GM, Cohen ML. A critical evaluation of the trigger point phenomenon. Rheumatol (United Kingdom). 2015;54(3):392-399. doi:10.1093/rheumatology/keu471
- Partanen J V, Ojala TA, Arokoski JPA. Myofascial syndrome and pain: A neurophysiological approach. Pathophysiol Off J Int Soc Pathophysiol. 2010;17(1):19-28. doi:10.1016/j.pathophys.2009.05.001
- Shah JP, Phillips TM, Danoff J V., Gerber LH. An in vivo microanalytical technique for measuring the local biochemical milieu of human skeletal muscle. J Appl Physiol. 2005;99(5):1977-1984. doi:10.1152/japplphysiol.00419.2005
- Shah JP, Gilliams EA. Uncovering the biochemical milieu of myofascial trigger points using in vivo microdialysis: an application of muscle pain concepts to myofascial pain syndrome. J Bodyw Mov Ther. 2008;12(4):371-384. doi:10.1016/j.jbmt.2008.06.006
- Ge HY, Arendt-Nielsen L, Madeleine P. Accelerated muscle fatigability of latent myofascial trigger points in humans. Pain Med (United States). 2012;13(7):957-964. doi:10.1111/j.1526-4637.2012.01416.x
- Ge H-Y, Zhang Y, Boudreau S, Yue S-W, Arendt-Nielsen L. Induction of muscle cramps by nociceptive stimulation of latent myofascial trigger points. Exp brain Res. 2008;187(4):623-629. doi:10.1007/s00221-008-1331-y
- Ibarra JM, Ge H-Y, Wang C, Martinez Vizcaino V, Graven-Nielsen T, Arendt-Nielsen L. Latent myofascial trigger points are associated with an increased antagonistic muscle activity during agonist muscle contraction. J Pain. 2011;12(12):1282-1288. doi:10.1016/j.jpain.2011.09.005
- De Meulemeester KE, Castelein B, Coppieters I, Barbe T, Cools A, Cagnie B. Comparing Trigger Point Dry Needling and Manual Pressure Technique for the Management of Myofascial Neck/Shoulder Pain: A Randomized Clinical Trial. J Manipulative Physiol Ther. 2017;40(1):11-20. doi:10.1016/j.jmpt.2016.10.008